If I know anything about viruses, it's that lots of folks overreact to them each and every time.
It's no secret the media frenzy has led to a crisis of misinformation. Much of that stems from a lack of knowledge and transparency. I already covered just how misleading the death reporting is. (You can reread that issue here.)
But no matter what the true death count is, you need to understand who is dying and who is most at risk. That's why last month, my team dug into the available data and helped demystify some of the misinformation. You can read the full issue of Retirement Millionaire here.
First of all, most people who wind up in the hospital (and most of those who die) are fighting more than just COVID-19.
We're seeing that many COVID-19 patients in ICUs have other infections as well. That means they've tested positive not just for the SARS-CoV-2 virus, but also for things like influenza and bacteria that classically cause pneumonia. Yes, these co-infections lead to more severe cases and deaths.
A small study out of China ran an antibody test on COVID-19 patients. It showed either current co-infections or infections they'd recently gotten over (which means their immune systems were still recovering) in 80% of COVID-19 patients. These people had biological markers of at least one other respiratory illness... and sometimes more than one.
For influenza, most deaths come from secondary infections like pneumonia. I suspect this remains true of COVID-19. Falsely reporting COVID-19 as the sole cause of every death is skewing the reporting.
Moreover, we know that poor health puts you at a higher risk of dying from COVID-19.
A study from Italy showed that more than 99% of deaths from COVID-19 happened in folks with other preexisting conditions. Nearly half of those deaths were people who suffered from three or more other conditions, like heart disease and diabetes. So again, I ask you... what really killed the patient?
A research team from the Brigham and Women's Hospital in Boston found that certain illnesses increased the odds ratio in COVID-19 deaths. In other words, your risk went up or down if you had certain factors...
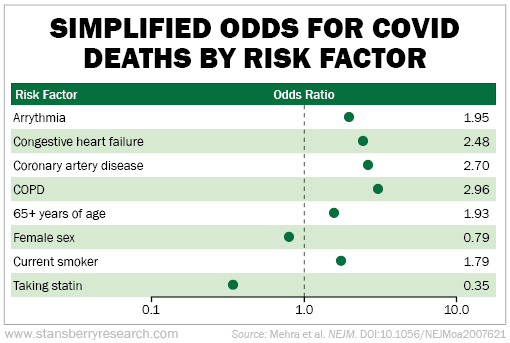
They looked at in-hospital deaths for folks with COVID-19. They found that conditions like chronic obstructive pulmonary disease ("COPD") made your risk three times higher. On the other end, women and those on statins had a lower chance of dying.
We also know that the virus attaches to a specific receptor, called angiotensin-converting enzyme 2 ("ACE2") in our bodies, many of which are in our lungs and heart. So preexisting issues with those organs increases your risk of complications and death as well.
And guess which group has the most preexisting conditions... Folks older than 65.
Recently, the Kaiser Family Foundation released a look at COVID-19 deaths and found something startling: More than half of all U.S. deaths so far are nursing-home residents.
We dug into the data from the U.S. Centers for Disease Control and Prevention ("CDC") last month and saw the trend fits. Of the 44,016 confirmed deaths from COVID-19 (again, likely inflated), 35,161 were folks age 65 and older. That's nearly 80% of all deaths from COVID-19 occurring in the oldest group of Americans. In fact, 31% of all deaths have been folks age 85 and older.
We already saw this pattern in Italy, one of the hardest-hit countries. Part of that had to do with its high population of older folks. And as we mentioned earlier, it's no surprise that over 99% of those who died had other conditions...
And a 2014 study from Italy found that about 86% of Italians over age 65 had at least one chronic health condition like high blood pressure, diabetes, or COPD. And 57% of those folks had more than one chronic condition.
This is why COVID-19 seems to be hitting nursing homes especially hard. It's preying on those who are already battling other illnesses and old age. So even if someone likely has little time left because of several severe health conditions, it's easy to write off their death as another COVID-19 victim.
This isn't the first flu season when Italy has struggled to keep up... Past research shows that the regular flu season each year sees a 51% increase in hospital patients, sending the hospital resources to max capacity. In bad flu seasons, like in 2017 to 2018, hospitals filled to the brim. Doctors, nurses, and ICUs were maxed out.
Around the world, governments have panicked, and people have died senselessly and without dignity... and apparently without much common sense. This terror over COVID-19 means doctors will force folks with little time left into hospitals, put them on ventilators (which can be a brutal experience), and leave them to die in a way that goes against their wishes.
Keep in mind, reporting has changed rapidly since we compiled this. Plus, each state reports their data differently - that's why it's so difficult to get the full picture on what's really going on. The best way to beat this pandemic is to arm yourself with information. That's why I urge you to tune in to my weekly COVID briefings with my senior analyst, Matt Weinschenk. You can find those here.
What We're Reading...
- Risk stratification for workers.
- Something different: Another consequence of the pandemic: Homesickness.
Here's to our health, wealth, and a great retirement,
Dr. David Eifrig and the Health & Wealth Bulletin Research Team
June 2, 2020
