It's still public enemy number one: Heart disease.
In the U.S., heart disease kills about 650,000 people each year. That's roughly 24% of all deaths.
Over the years, I've written several times about the importance of heart health. But this month I'm going a step further...
February is National Heart Month. So, throughout the month, we're going to highlight heart health in several issues of Health & Wealth Bulletin.
Today we're starting with the "Silent Killer"... high blood pressure.
High blood pressure earned this nickname because symptoms often emerge too late to avoid dire (even fatal) health consequences. One of the first signs can be a stroke.
That's why regular screenings are lifesaving.
Blood pressure screening is one of the tests I often recommend. It has earned an A rating from the U.S. Preventive Services Task Force (USPSTF). This is the panel that looks at evidence for screenings, counseling services, and preventive medicine. They assign grades based on the strength of the evidence that these screenings have a high net benefit.
Screening is pretty standard. At any doctor's visit, it's one of the vitals they take. A blood-pressure monitor usually involves a cuff that goes around your arm and inflates and deflates. It measures the pressure in your arteries when the heart beats (the top number) and the pressure in between beats (the bottom number).
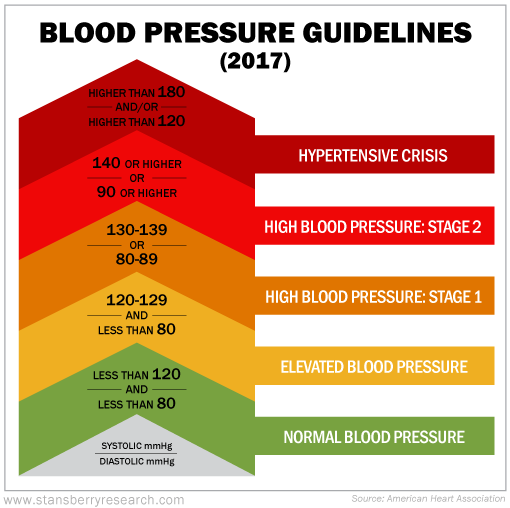
It used to be that high blood pressure just meant a reading that was 140/90 mm Hg or higher. But a few years ago, the American Heart Association, along with a few other heart health groups, evaluated new evidence regarding treatment. They lowered the threshold down to 130/80 mm Hg instead.
In other words, 31 million folks suddenly had high blood pressure overnight.
The changes were a bit more nuanced than that though... They included getting rid of the "prehypertension" category and broke out high blood pressure as Stage 1 and Stage 2. There's now an elevated category instead of "prehypertension." The idea is that "prehypertension" folks now have a more serious diagnosis, which could prompt them to be more proactive about lowering their blood pressure.
Initially, we worried that the change in guidelines was a ploy to push for more blood pressure meds. And in some cases, that might happen. But we've also seen several doctors write about how the new guidelines simply give them more power to urge diet and lifestyle changes.
That's great news since we already think folks are over-medicated for problems that they can actually fix on their own.
There are some factors that temporarily elevate blood pressure, so be sure to follow these five rules when you get yours measured.
- Sit with your feet on the floor.
- Don't drink caffeine beforehand – depending on your tolerance, you may want to stop drinking it 30 minutes to a few hours before.
- Take deep breaths and try to relax.
- Don't talk.
- Make sure you're hydrated. Chronic dehydration elevates blood pressure and many folks (seniors in particular) are terrible at drinking enough water. Be sure to drink about six to eight glasses a day.
If you're at the doctor's office and follow these steps but still have high blood pressure, ask to have them take your pressure again at the end of the appointment.
That's because of something called "white coat syndrome." This happens when you experience stress or anxiety from going to the doctor. The sight of a "white coat" (like the kind doctors wear) is enough to stress you out and raise your blood pressure.
If you're in the elevated or Stage 1 level, talk to your doctor about making lifestyle changes instead of taking medication. For stage 2, you may need medication, but talk about making these changes and retesting at a follow up appointment to see if you can stop taking the meds in the future.
1. Make sure you follow healthy lifestyle guidelines. Exercise regularly – at least 30 minutes, five days a week. I like to take a 30-minute walk every day to get my exercise in. Eat more vegetables (especially green, leafy veggies), fish, and whole foods. Cut out fatty foods and what I call "white killers" (white flour, white potatoes, and white sugar). Some foods that reduce blood pressure are dark chocolate, eggs, wine, olive oil, and foods that are high in potassium.
And don't forget this type of salt... magnesium. Many folks experience problems with blood pressure because they don't get enough magnesium. So be sure to include nuts, seeds, and leafy greens in your diet.
2. Keep track of your blood pressure. Start a log of your blood-pressure readings. Write your test results down at the doctor's office. If you get a high-pressure reading, wait a few days and try it again.
Fortunately, you don't need to spend time at a doctor's office to monitor your blood pressure. Many stores like Rite Aid, Walgreens, and many Walmart pharmacies have blood-pressure monitors in the store. I regularly roll up my sleeve and use these monitors to check my blood pressure.
You can also buy a blood pressure monitor and take readings yourself. Just be sure not to use a fingertip or wrist model – these aren't accurate and may give wildly different readings in just a few minutes.
3. Finally, do what I do – meditate regularly. This can quickly relieve sensations of stress. After a few months of regular meditation, research shows you can lower your blood pressure by at least 10 points without visiting a doctor or using medications. Try meditating before getting your blood pressure checked as well... and even during the test itself. The results will surprise you.
Managing your blood pressure is a great way to take charge of your heart health. Making practical lifestyle changes like dieting, exercising, and managing stress will keep you and your ticker in good shape.
What We're Reading…
- A deeper look at the new guidelines.
- Something different: How do buffets make money?
Here's to our health, wealth, and a great retirement,
Dr. David Eifrig and the Health & Wealth Bulletin Research Team
February 4, 2020