221 million prescriptions...
That's the latest number available for the number of prescriptions written in a single year (2012-2013) for statins.
In a little more than a decade, from 2002 to 2013, use of this cholesterol medicine increased 80%. The reason? The American Heart Association lowered the guidelines for "normal" cholesterol numbers. Overnight, millions of Americans suddenly had high cholesterol... and doctors turned to Big Pharma to "fix" the problem.
Today, one in four Americans over the age of 40 takes statins. That number makes my blood boil. Particularly when friends of mine resign themselves to taking the drug for the rest of their lives.
I've written before about the big myth behind cholesterol. Solely treating a set of numbers with an overprescribed drug class like statins is an irresponsible – and dangerous – practice.
That's largely due to the fact that inflammation – not cholesterol – is the root cause of heart disease. That's why simply treating cholesterol numbers doesn't work. Doctors need to focus on the whole patient – including lifestyle elements like diet and exercise.
But given how many folks still write to me asking about statins, I wanted to address my views on them in today's issue. Let's get started...
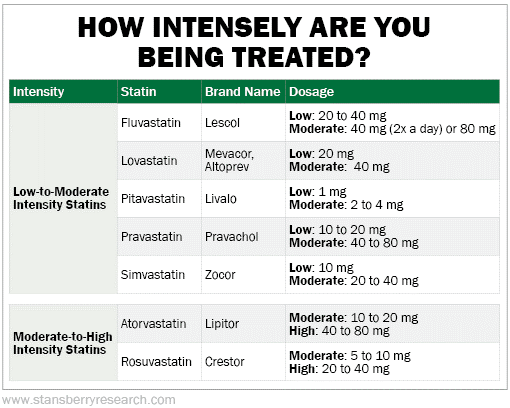
What Are Statins?
Statin drugs work directly with the liver. They effectively stop the work of an enzyme called HMG-CoA reductase. This enzyme controls the liver's production of low-density lipoprotein (LDL) cholesterol – the so-called "bad" cholesterol. When the liver stops making LDL, your body scavenges it from your bloodstream and elsewhere (since you still need LDL for important bodily functions, like breaking down your food with bile inside your gut).
But there's a big problem with statins. For years, Big Pharma funded the safety studies. Many of those early studies showed that statins lowered early mortality rates from heart disease. But this is like letting 12-year-olds buy whatever they want in the candy section.
In 2005, the scientific community changed how it reported clinical trials after it was discovered that severe adverse effects in popular painkillers Vioxx and Celebrex had gone unreported. According to a 2015 paper from the World Journal of Cardiology, this was the turning point – since then, no paper on statins has shown a significant change in mortality rates. Oops.
To illustrate this, an analysis done by the gold-standard reviewing group Cochrane looked at hundreds of statin papers. The group reviewed about 250 studies on atorvastatin in different doses. The lowest dose (2.5 mg) was reported to lower LDL numbers by about 25.2% and the highest dose (80mg) lowered them by 53.5%. And triglycerides reduced 11.6% for the lowest dose versus 32.1% for the highest dose.
Now, that sounds fantastic. But there are a few problems. As the Cochrane review points out, atorvastatin manufacturers funded more than half of these studies. They also ran the studies for only about three to 12 weeks. That's not nearly enough time to get a real look at the safety profile for a drug.
Another big trial, called the JUPITER trial, looked at rosuvastatin as a primary prevention medication. (That means giving it to folks who haven't had a heart attack yet – they just have elevated cholesterol numbers.)
The problem with JUPITER was that it reported a 44% reduction in heart attacks... but that's misleading. The absolute risk reduction – which measures real-world results of the medical intervention – was a little more than 1%.
These results are abominable. Further studies show that at best, only about half of folks on one type of statin (rosuvastatin) saw their cholesterol levels drop to the "targeted" goals. And the results for other statins fared far worse.
That's because these drugs don't work alone. Instead, you need to change your lifestyle to lower your risk of heart disease. As a reminder, our top three lifestyle changes are:
- Eat the right foods. Avoid trans fats, processed foods, and other inflammation-triggering foods.
- Eat the right way. Try mindful eating as well as fasting.
- Exercise. High-intensity interval training (HIIT) is an efficient way to not just fight inflammation, but also to help burn inflammation-triggering excess fat.
By now, I hope you begin to understand my reservations with statins. Not only do we lack any long-term statin studies on safety and efficacy, we do know they carry severe side effects.
Next week, I'll dive into what those side effects are. Plus, I've got a list of things to discuss with your doctor should he recommend statins for you. You won't want to miss that issue!
What We're Reading...
- Finally, some research on how statins cause muscle pain.
- Something different: Stop badgering us...
Here's to our health, wealth, and a great retirement,
Dr. David Eifrig and the Health & Wealth Bulletin Research Team
September 17, 2019
